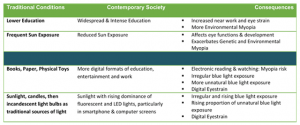
The past 3 decades have involved widespread technological and lifestyle changes, many of which have critical consequences for eye health. Aside from changes that we now realise have contributed to an epidemic of myopia (shortsightedness), the changes to learning and entertainment, namely consistent use of electronic devices for reading and watching, may be leading towards more prevalent and rapid macular degeneration.
The theorised culprit is blue light (380nm – 500nm), or more specifically, blue-violet light (380nm – 450nm). This is a range of light within the visible light spectrum (380nm – 780nm) which is of short wavelengths and therefore high energy. In fact, this range is adjacent to ultra-violet light, which is well known for causing skin cancer and cataracts when a person is over-exposed.
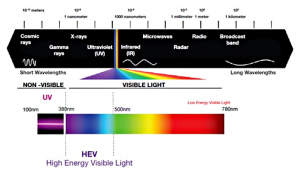
Source: Essilor of America Inc. (2013). The electromagnetic spectrum and optical radiation.
Attesting to the potency of these light waves, current scientific applications and research include treating inflammatory acne and potential use as a disinfecting agent, which “can photo dynamically inactivate the cells of a wide spectrum of bacteria”[1] including MRSA, E. Coli and H. Pylori.[2] Blue light’s validity in treating wound infections is because it does less damage to mammalian cells than its neighbour, UV light. However, the unique characteristics of the eye must be considered:
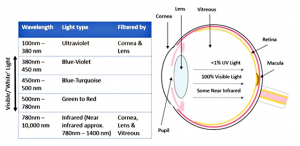
Light reaching the retina’s rods and cones comprises human sight. The primary source of light is of course sunlight, and the full range of it is filtered through the Earth’s atmosphere and several structures of the eye before it reaches the retina. Owing to the functioning of the cornea and lens, less than 1% of UVA and UVB reach the back of the eye. The next layer of defence, the vitreous humor, then filters out most of the infrared light, beyond the range of 1400nm. As a result, these two small proportions of UV and infrared, with all wavelengths in between, reach the retina. We perceive the ‘visible light’ as colours according to the amount of energy (frequency) matched inversely to their wavelengths. The macula, a ‘yellow spot’ situated near the optic nerve is the primary receiver of these types of light.
While the primary source of blue light was the sun (hence its influence on circadian rhythm), the increase in exposure to unnatural blue light sources like LED-lit rooms and screens has consequences for both the sleep-wake cycle and eye health, particularly of the macula. This could be all the more so since we gaze directly at smartphone, computer and television screens, which are made with “cold white LEDs” that emit 30% blue light.[3] This format of exposure ensures that the unfiltered bands of emitted blue-violet light end up directly within central vision and therefore, the macula.
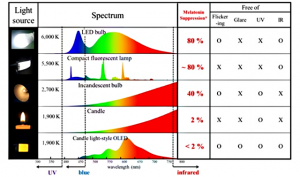
Source: Jwo-HueiJou and Chun-Yu Hsieh (2013)
The <1% of UV and the adjacent band of blue-violet light are the highest energy components of light reaching the retina, and the natural suspicion is: If we know that UV can cause eye damage, what can the band of blue-violet light (with similar energy characteristics) do to the sensitive cells at the rear of the eye, given the exposure conditions of contemporary society?
Essilor partnered with the Paris Vision Institute to investigate the effect of blue light on animal eyes, using the Retinal Pigment Epithelium tissue. The results showed that the band of wavelengths between 415nm to 455nm caused the largest number of destroyed cells via apoptosis. The RPE cells were described as undergoing “cell rounding, loss of confluence, and decrease of density” within 6 hours of exposure.[4] A 2005 study also found that bands of 408nm and 430nm caused “massive lesions” in the retina tissue used. Within 2 minutes or less of exposure, lesions of the RPE and “irreversible death of photoreceptors” resulted. However, when the cells were treated with green light, there were was no structural change or damage.[5]
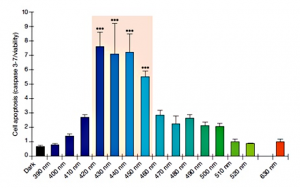
Source: Essilor of America Inc. (2013)
‘Apoptosis’ is referred to as programmed cell death, or even ‘cell suicide’, and is a naturally occurring internal process with roles in cell renewal and system defence, including destruction of damaged and potentially cancerous cells. This is opposed to ‘necrosis’, which tends to occur as a result of exposure to external chemicals or poison. The higher rates of RPE cell suicides observed in the first study partially explain acceleration of age-related macular degeneration, which involves the death of photoreceptor cells in the macula without replacement. As the RPE provides a vital support system for the rods and cones, damage to the cells within the RPE has grave implications for photoreceptors and vision.
While scientists are so far uncertain about the mechanisms involved and the long-term effect unnatural blue-violet light has on human eyes, for the time being and given initial research, it seems reasonable to err on the side of caution.
References and Further Resources
[1] Halstead, F. D. (2016). Antibacterial Activity of Blue Light against Nosocomial Wound Pathogens Growing Planktonically and as Mature Biofilms. Applied and Environmental Microbiology 2016 July; 82(13): 4006-4016. http://aem.asm.org/content/82/13/4006.full
[2] Effect on MRSA covered in Enwemeka, C. S. et. al. (2009).Blue 470-nm light kills methicillin-resistant Staphylococcus aureus (MRSA) in vitro. Photomedicine and Laser Surgery. 2009 April; 27(2):221-226
Effect on E. Coli covered in Lipovsky et. al. (2010). Visible light-induced killing of bacteria as a function of wavelength: implication for wound healing. Lasers in Surgery and Medicine. 2010 Aug;42(6):467-72
[3]Barrau, C. (2014). The Back: Blue Light and Eye Health. Shedding light on this spectrum and eye health.Optometric Management.2014 March;49: 30-32.http://www.optometricmanagement.com/issues/2014/march-2014/the-back-blue-light-and-eye-health
[4] Blue Light Hazard: New Knowledge, New Approaches to Maintaining Ocular Health. REPORT OF A ROUNDTABLE
March 16, 2013, New York City, NY, USA. Sponsored by Essilor of America Inc.
http://www.crizalusa.com/content/dam/crizal/us/en/pdf/blue-light/Blue-Light-Roundtable_White-Paper.pdf
[5]Reme, C. E. (2005). BLUE LIGHT AND THE RETINA: GOOD AND BAD?
The role of lutein and zeaxanthin: https://www.macular.org/study-demonstrates-essential-role-zeaxanthin-eye-health
Effect on Insulin Resistance: http://journals.plos.org/plosone/article?id=10.1371/journal.pone.0155601#sec013
http://www.bluelightexposed.com/#blue-light-and-macular-degeneration
https://www.reviewofoptometry.com/ce/the-lowdown-on-blue-light-good-vs-bad-and-its-connection-to-amd-109744
https://medium.com/@jasonlauritzen/blue-light-and-health-plus-how-to-make-your-own-blue-blocking-glasses-1a3d2694ad60#.govdwr361
Różanowska, M. and Sarna, T. (2005), Light-induced Damage to the Retina: Role of Rhodopsin Chromophore Revisited. Photochemistry and Photobiology, 81: 1305–1330. http://onlinelibrary.wiley.com/doi/10.1562/2004-11-13-IR-371/full
Gringras, P. et. al. (2015).Bigger, Brighter, Bluer-Better? Current light-emitting devices – adverse sleep properties and preventative strategies. Frontiers in Public Health 2015 October; 3: 233. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4602096/
Risk Factors of Blue and Bright Light Therapy. (Sunnex Biotechnologies: Winnipeg, Canada) http://www.sunnexbiotech.com/therapist/blue%20light%20damage.html








